How Unity Health teams are bringing COVID-19 vaccines to homebound patients

Elizabeth Niedra, family physician and homebound vaccination team lead, and Shawna Irons, family physician, head out on the road for a day of homebound vaccinations in West Toronto.
Individuals who are homebound face significant barriers to receiving a COVID-19 vaccination. Though these individuals aren’t able to leave home for a variety of reasons, they can still be exposed to the virus through the family members, friends or support workers who care for them. Often those who are homebound are elderly or have health conditions that put them at higher risk of becoming severely ill with COVID-19.
Dr. Amy Freedman and Dr. Elizabeth Niedra are primary care physicians who practice in the home visiting programs for the frail elderly with St. Michael’s Academic Family Health Team and St. Joseph’s Urban Family Health Team, respectively. With their extensive background in primary care home visiting, they have taken on the physician lead roles for the homebound vaccination programs at Unity Health, which has administered nearly 1000 vaccines so far. They joined us to talk about their work and why it’s critical to reach the hard to reach.
What would make someone eligible for a homebound vaccination?
EN: We’ve been very thoughtful about the referral criteria and it’s been really rewarding to reach a lot of people who – for many different reasons – would face barriers getting out to a vaccine clinic.
AF: Either for physical or mental health reasons or because of social vulnerability – it’s really people who can’t access a vaccine clinic and their caregivers that we are focused on.
EN: We have an age cut-off of 18 years of age and older. We are using the Moderna COVID-19 vaccine – as it’s much easier to transport – and it’s only been approved for those 18 years of age and older.
AF: It’s also important to note that there are six homebound vaccine outreach teams in the GTA and we work collaboratively to cover the city. Our programs run in the West and Downtown East.

How does someone get a referral to the homebound vaccination program?
AF: At St. Michael’s we’ve gone through different iterations. At first we piloted with referrals from our family health team. We then opened it up to the Downtown East family physicians. And then we expanded it to many of the agencies in the Downtown East community – places like Woodgreen and Fred Victor.
EN: I think the success story of our team so far is that we’ve exhausted the referral pool of the West Toronto primary care groups. I think the Downtown East is in a similar situation.
When we first started this back in March the idea was that all the homecare patients in the Toronto Region Local Health Integration Network would be vaccinated by the Emergency Medical Services paramedics. It soon became clear that it was going to take some time to work through those lists. So we’ve helped to support that team by taking on patients on that list who fell within our catchment.
For the people who we can reach – who are connected to a family doctor or a community agency – our sense is that we’ve actually found those people. But there are many more who don’t have those traditional connections – that’s the next challenge that we need to figure out.
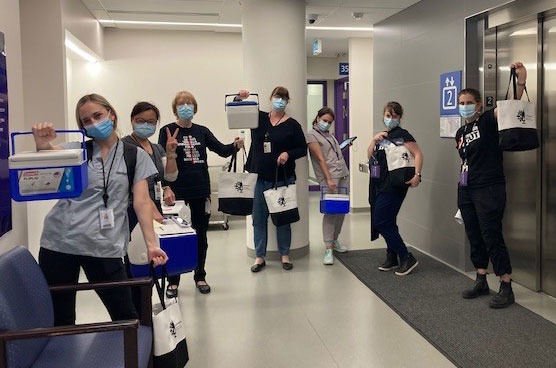
The homebound vaccination team at St. Michael’s prepare for a day on the road (Left to right: Jessica Cuppage, family physician; Doret Cheng, clinical pharmacy practitioner; Lorna McDougall, nurse practitioner (NP); Laurie Green, family physician; Nicole Deziel, NP student; Kari Fulton , NP; Amy Freedman, family physician and homebound vaccination team lead)
What does a day in the life of a homebound vaccinator look like?
EN: We’ll meet in the morning at the hospital with all the other vaccinators and a pharmacy technician. The pharmacy technician will pre-draw up all the doses we need from a list that our dispatcher – or administrative person – will send them the night before. They are all ready to go – pre-packaged in coolers with cooler blankets. We also have a little toolkit with all our vaccination supplies.
Then we will map out our routes through the city for the day with the list of homebound individuals we are going to see.
We stay in touch throughout the day so while we’re on the road, if we run into any trouble – whether it’s with the technology we’re using, or you go to see someone and they have COVID-19 symptoms so they aren’t currently eligible, or we aren’t able to get consent, or someone isn’t home – we can contact the rest of the team and get re-assigned a new patient and bring that dose to them.
It’s very on the road and on the fly and collaborative.
AF: There is a huge amount of logistics that go into planning that day. The patients are carefully selected to be within a certain geographic area because it’s critical that we don’t waste a single dose – and we have to use the vaccines within those six hours.

A cooler pre-packaged with doses of Moderna ready for a day of homebound vaccinations.
What are some of the key takeaways you’ve had from this experience?
EN: This experienced re-emphasized for me that you are always going to need nuanced and gentle solutions for these really vulnerable patients – because you won’t always catch them in those big sort of “blitz” operations.
You need to be on-the-ground and community-based. Without this kind of work, people do fall through the cracks and the pandemic has really emphasized that for us.
AF: One of the really lovely things for us is that we’ve had all these family doctors acting as vaccinators who haven’t previously been doing home visits – and they love it! There is something very rewarding and meaningful about going into people’s homes and offering them a vaccine and some hope for the end of this pandemic.
Why is this program so important?
EN: On the surface, we are giving out such small numbers of doses compared to the huge programs and clinics that do thousands of vaccines a day. But every one of these vaccines truly counted – and you can see that in the whole context of visiting people at home.
This work is incredibly resource-intensive and we have no idea how many potential COVID-19 cases and deaths we are preventing – but every hospitalization and death prevented is significant.
AF: We heard in New York City that in the intensive care units they were actually seeing a lot of homebound, unvaccinated patients. We know that many of the homebound patients are elderly and have complex medical illnesses. These hard to reach patients would have very poor outcomes from COVID.
EN: They are hard to reach for us but they often have so much contact with personal support workers, nurses, family members and neighbors. The purpose of this team is to fill in the gaps for these actually high risk people, and be that hand that can reach the hard to reach.
Final thoughts?
AF: This has really been a team effort – the pharmacy team, the administrative team, the nurses, nurse practitioners, the family physicians. We’re very grateful to have their support.
EN: I’m from West Toronto. I was born here, grew up here and I work here now – it feels good to give back to my community.
If you have questions about Unity Health’s homebound vaccination programs in the West and Downtown East, please reach out to communications@unityhealth.to.
By: Robyn Cox
