St. Michael’s Hospital team performs first-in-Canada minimally invasive neurovascular procedure
What to know:
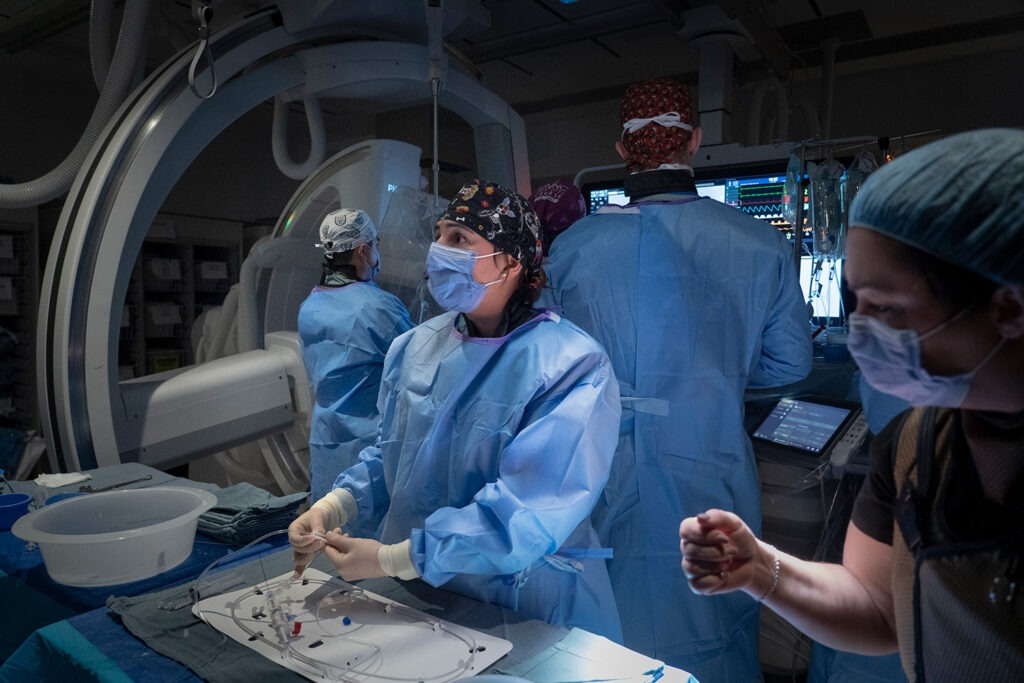
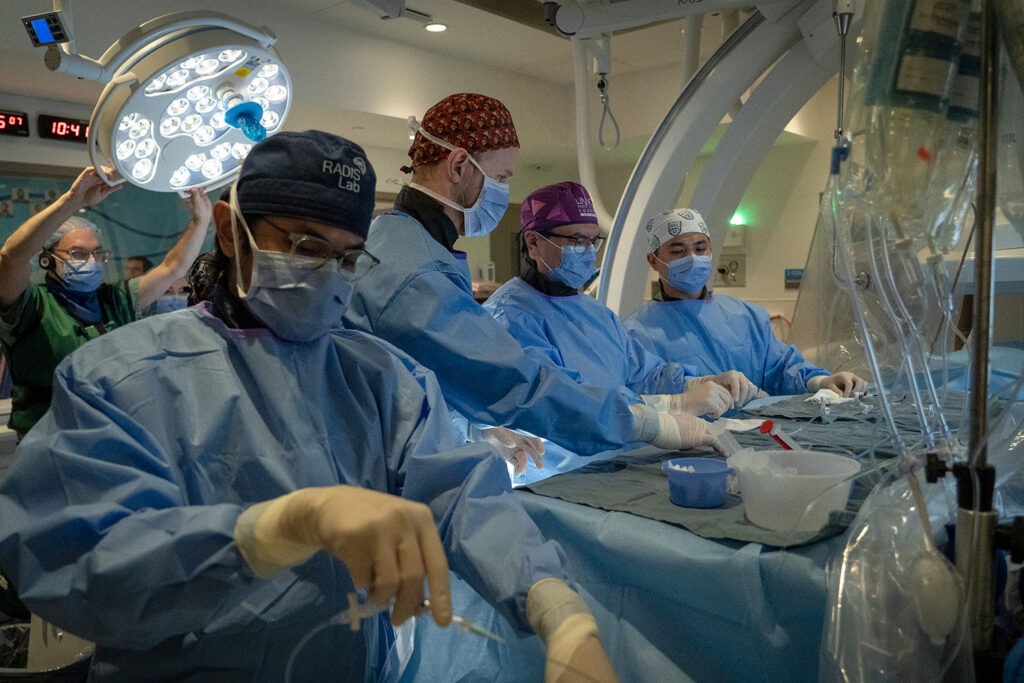
- Dr. Vitor Pereira, a neurosurgeon at St. Michael’s Hospital, led a team to complete the first eShunt® Implant procedure in Canada.
- The implant is a treatment option for Normal Pressure Hydrocephalus (NPH), a condition that affects more than 1 in 200 adults over the age of 65 and causes difficulties with balance, bladder control, thinking and memory due to fluid build up in the brain.
- Dr. Jose Danilo Diestro, an interventional neuroradiologist, did the procedure alongside Pereira and continued to care for the patient, Abdul Rehman, afterwards.
- The implant is the first minimally invasive surgical option for NPH, which has the potential to reduce hospital stays and create opportunities for patients who would not be able to receive more invasive surgeries.
- The eShunt System is currently being studied for safety and efficacy in the STRIDE Clinical Trial.
- Learn more about this case in this story from CTV News.
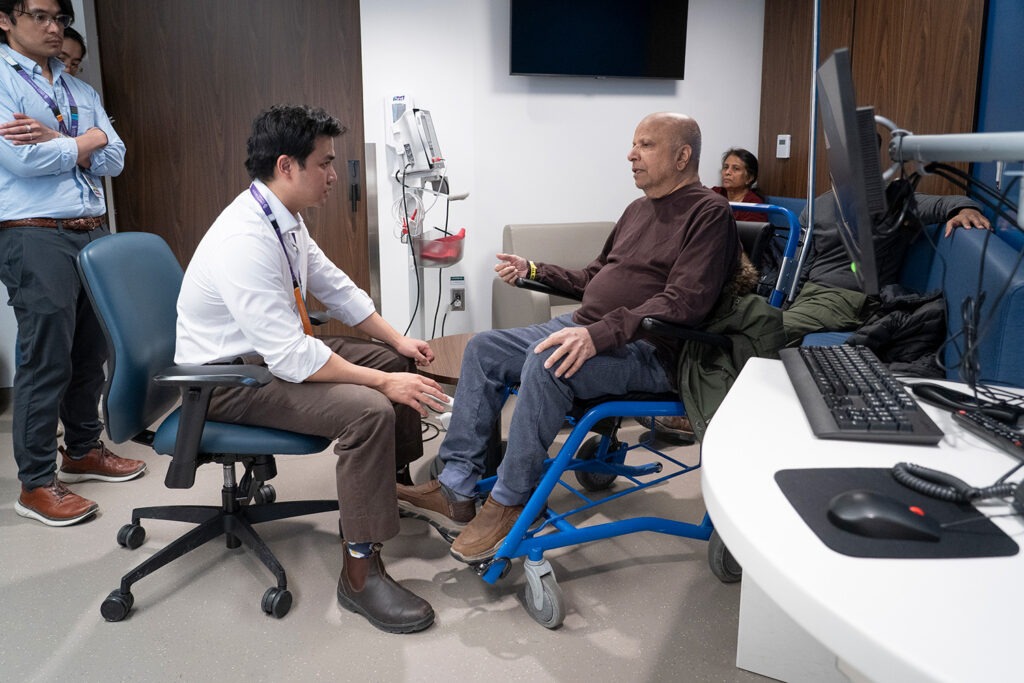
It’s been six weeks since Abdul Rehman’s brain surgery. He sits in the clinic room with his wife, Subaida, and their son, Manzar, waiting to have a conversation with his vascular neurologist. The procedure has gone well, and Rehman and his family are beginning to see improvements.
When Dr. Jose Danilo Diestro walks in, he and the family exchange greetings and smiles. The family asks questions – they have begun to see increases in his cognitive ability and mobility and are curious about how things will continue to progress.
Diestro assures them that improvements take time and with continued rehabilitation, Rehman will continue to make gains.
“When I speak to his wife and his son, they feel like he’s doing better in terms of mobilizing and climbing stairs,” says Diestro. “When I met with him today, he was different. He was much brighter than what I remember – aware of what’s going on around him and speaking up more.”
A Canadian first
Rehman is the first in Canada to have the eShunt® Implant placed in his brain. This implant is a potential treatment option for patients who have Normal Pressure Hydrocephalus (NPH), a condition where fluid builds up in the brain and puts pressure on nearby brain tissue. It causes difficulties with balance, bladder control, thinking and memory.
NPH affects more than 1 in 200 adults over the age of 65 and is often mistaken for other conditions like Alzheimer’s disease, Parkinson’s disease or general cognitive decline associated with aging.
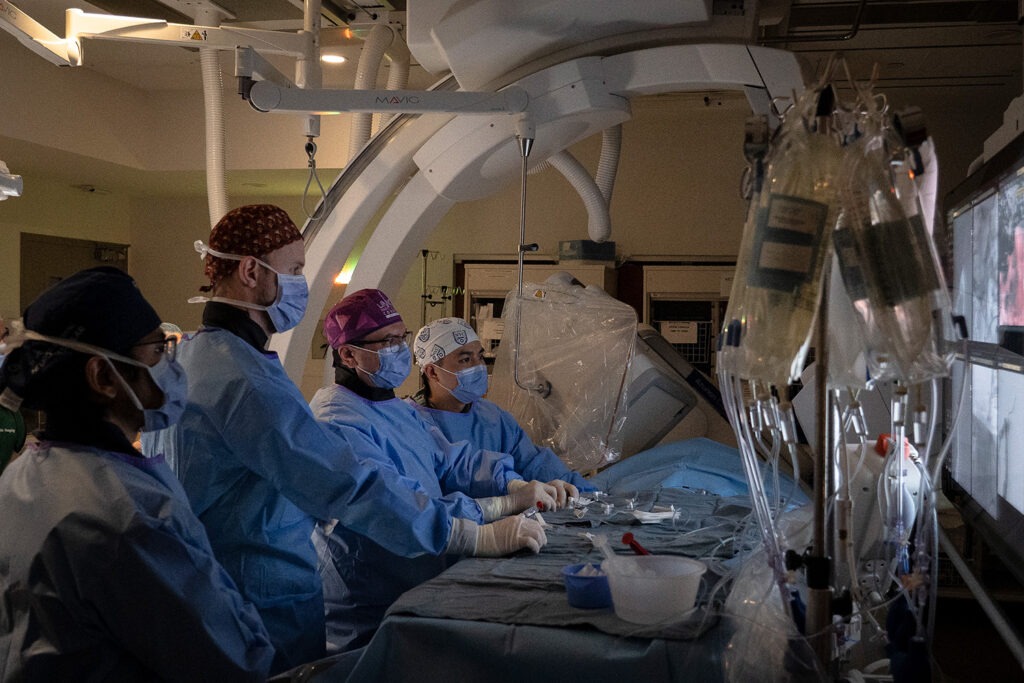
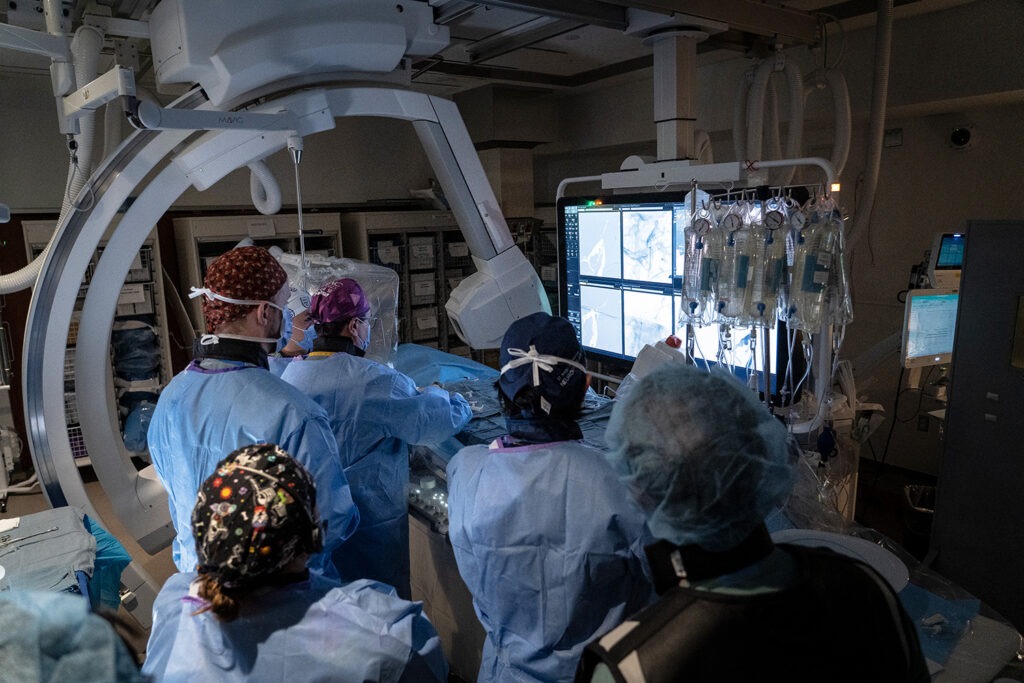
The surgery was led by Dr. Vitor Mendes Pereira, neurosurgeon and lead scientist of the RADIS Lab at St. Michael’s Hospital and professor with the Department of Surgery at the University of Toronto. The RADIS lab uses advanced technologies to improve outcomes for patients with neurovascular diseases. Diestro, who specializes in interventional neuroradiology, did the procedure with him and continues to follow Rehman’s progress. Interventional neuroradiology is the use of minimally invasive, image-guided technologies to treat vascular diseases of the brain, neck and spine.
The current standard of care for patients with NPH is to use a ventriculoperitoneal (VP) shunt, which is placed in the brain during open brain surgery. Both shunts help to drain excess fluid from the brain to another area of the body where it can be reabsorbed. With both shunts, patients can expect to see improvements in their balance and mobility, cognitive skills and bladder control.
The eShunt System is manufactured by CereVasc, Inc. and is currently being studied for safety and efficacy in the STRIDE Clinical Trial. St. Michael’s Hospital is the first Canadian site participating in the STRIDE Clinical Trial and Dr. Pereira is the principal investigator, which means he’s the lead researcher responsible for the clinical trial at the hospital.
“VP shunting remains the standard of care, but its limitations are well recognized, with up to 25 per cent of patients experiencing complications or requiring revision within the first two years,” says Pereira. “This has driven a long-standing need to rethink how we treat these patients and to develop less invasive, more reliable solutions.”
Opening doors with minimally invasive treatment
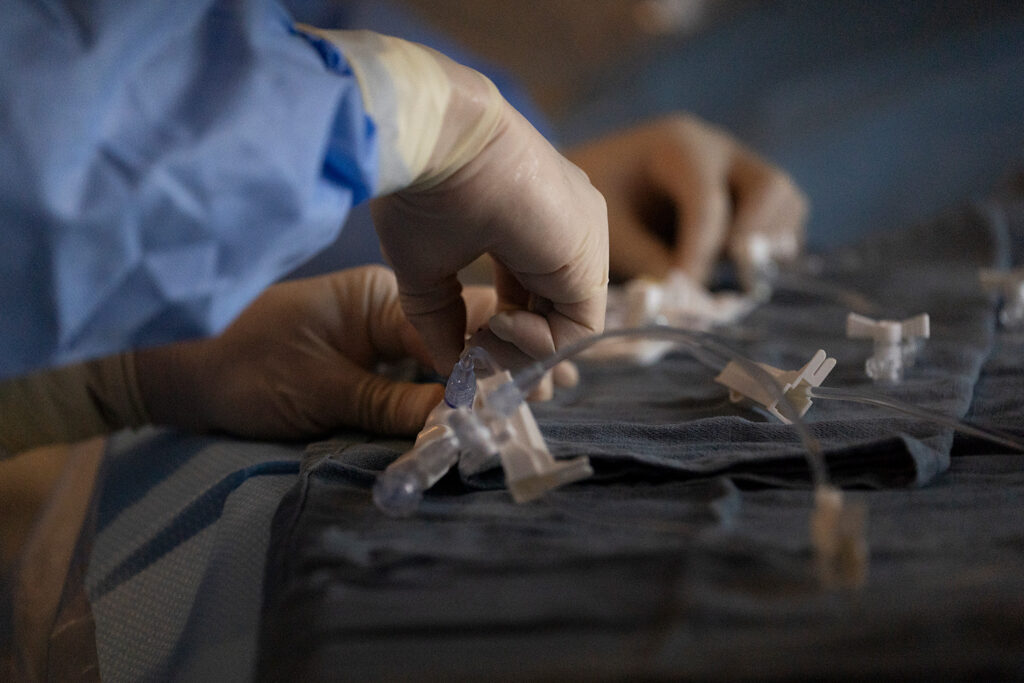
What sets this treatment apart is that it’s minimally invasive. The implant is placed in the brain through blood vessels, requiring only one vascular access near the groin. This means patients can expect to stay only one night in hospital after treatment, whereas a patient receiving a VP shunt can expect to stay in hospital for two to four days.
The minimally invasive nature of the procedure also creates opportunities for patients who would not be able to receive a VP shunt because of other health conditions.
“If effective, this approach could expand treatment to patients who are not candidates for traditional surgery due to high risk,” says Pereira. “This includes those on anticoagulation, with abdominal disease or in acute settings like the ICU, where a complex operation or transfer to the operating room may not be possible.”
Motivated to improve patient outcomes
Pereira’s research and clinical work with the RADIS lab is focused on using the latest robotic, minimally invasive and AI technologies to achieve better outcomes for people with neurovascular conditions. He is regularly on the cutting edge of new treatment technologies – performing several clinical firsts at St. Michael’s Hospital and abroad.
“I’ve always been intrigued with, first, cases that I couldn’t treat or understand and, second, better, less invasive ways to treat diseases,” says Pereira. “I’m always thinking of how I can do better, how I can teach better and if there is a new way to treat a disease that will make the treatment more consistent, safer and more accessible.”
Diestro is a vascular neurologist and has a strong passion for his specialty of interventional neuroradiology. “I’m motivated by the rush I get doing a very acute, life-saving procedure. For example, one of the most impactful procedures for patients is mechanical thrombectomy. You can have a patient who is unable to move one side of their body and the following day they are practically walking out of the hospital.”
Pereira and Diestro’s combined experience and motivation to do all they can for their patients is what draws them to clinical trials like the STRIDE trial.
“In clinic, the RADIS lab team and I will see a clinical problem. We bring it to the lab, we brainstorm, we apply for grants, we develop research and we partner with companies,” says Pereira. “When we see that it’s something that can potentially be translated to patients, we organize or join a clinical study. We pursue curiosity and exploration to make a positive impact for patients.”
Hopes for the future
Rehman’s NPH symptoms were first investigated after he experienced a fall. As is often the case with NPH, it took time for him to receive a diagnosis. NPH has similar symptoms to other conditions affecting older people – such as issues with balance, memory and thinking – and there is a process to rule out other concerns.
Now that he has received his new shunt and has started his recovery, he and his family hope to return to some of the cherished activities they used to enjoy – like walks, playing with their grandchildren and other family events.
“We used to go on walks, Abdul and I,” says Subaida Rehman. “We liked going out and enjoying the weather or strolling around the mall. I hope we can get back to that.”
By Robyn Cox
Photos by Kevin Van Paassen