Four years and 66 surgeries: How St. Michael’s Hospital became “home” to a patient
BY OLIVIA LAVERY
VIDEO AND PHOTOS BY KEVIN VAN PAASSEN
Benjamin Finlan is late for our interview, but not because he lacks time management. Everywhere he goes at St. Michael’s Hospital, he’s stopped by people who want to hug him: at the Tim Hortons in the Peter Gilgan Patient Care Tower, outside a meeting room in the Li Ka Shing building, and in the Trauma & Neurosurgery Inpatient Unit.
He’s not an easy person to forget; tall, personable, and warm. And even without his trademark charisma, the staff and care teams at St. Michael’s would know him anywhere. After all, he lived at the hospital for four years.
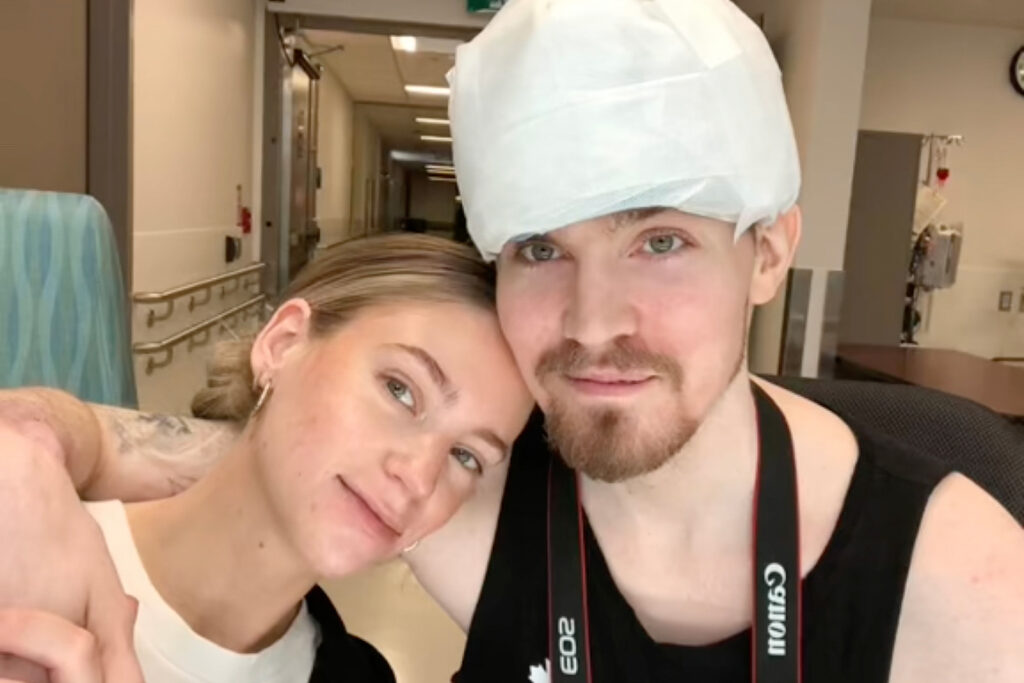
In early December 2018, at the age of 28, Ben was badly injured in an unprovoked attack while in London, England on a trip with friends. His skull was fractured in several places, and the result was a traumatic brain injury (TBI).
The events on the night of Ben’s injury launched a medical odyssey that spanned two continents and many years, taking him from ambulances to airplanes to operating rooms and intensive care units and, finally, home.
Enjoying this story? Sign up for the Unity Health Toronto newsletter, a monthly update on the latest news, stories, patient voices and research emailed directly to subscribers.
Ultimately, Ben required 65 surgeries over four years to reconstruct his skull, fend off complications, and get him back on his feet.
What Ben needed was a system of seamless, wraparound care that would provide everything from surgery to mobility and speech therapy.
“I thought of hospitals so differently before my injury happened,” says Ben. “I thought it was like: emergency department, surgery, in for a week max, and then out and back home.”
“The goal was to keep him alive.”
Ben’s girlfriend, Katherine Smith, was 25 years old when Ben was attacked. She was getting ready for work when Ben’s mom called to tell her that he had been badly injured. She got on the first flight from Toronto to London.
“We were going there under the impression that we were going to say goodbye,” she says. “They didn’t think he was going to survive the night. It seemed the goal was to keep him alive so we could have our final moment with him.”
Video: Ben’s story
Against the odds, Ben survived the night. After several days in a coma, his condition improved. Katherine and Ben’s family spent a few weeks in London, and eventually Ben was cleared to fly home.
By this point, part of Ben’s skull had been removed to allow his brain to expand and swell. He had contracted meningitis while in England, and was still on antibiotics. Upon arrival in Canada, he spent several days at St. Michael’s Hospital for quarantine, stabilization and monitoring, a common practice for patients who are returning home from another country.
As a Level 1 Trauma Centre, verified by the American College of Surgeons, St. Michael’s Hospital is equipped to provide the most advanced care to critically injured patients from across Toronto and well beyond. It is home to Ontario’s largest head injury clinic, and also to a number of surgeons, physicians, staff and scientists who have dedicated their careers to studying the brain from every angle to find the best treatments for patients with head injuries, brain cancer, neurodegenerative disease, and more.
Spencer McClung was one of the first nurses Ben and Katherine met when they arrived at St. Michael’s. McClung says he was immediately struck by how sick Ben was, but also impressed that his family had managed to get him across an ocean.

“It was quite a dramatic entrance,” McClung says, remembering how Ben’s mom pushed him through the elevator doors in a wheelchair.
The priority in those first few days was to make him comfortable and start providing basic care. After being stabilized, Ben went to a rehabilitation centre, with the plan being to give him time to get well enough to be able to do his skull replacement surgery in a couple of months.
At first, things seemed to be going well at rehab. Ben was still defying all of the expectations of the people and medical professionals around him. Then things took a sharp turn.
Because Ben’s skull had been removed, the skin on his head had started to cave in and put pressure on his brain. His function declined so rapidly that he was rushed back to St. Michael’s. It quickly became clear that he wouldn’t be going home any time soon. Katherine, now 26, quit her job to become his full time caregiver.
Brain Injury Canada reports that two per cent of the Canadian population lives with a TBI. According to the Canadian Hospitals Injury Reporting and Prevention Program (CHIRPP), which collects clinical data on emergency department visits from 21 hospitals across Canada, there were 650,336 TBIs from April 1, 2011 and February 12, 2024.
TBIs are painful not only for the people who endure them, but everyone who loves them as well. Symptoms like memory loss, personality changes and seizures can profoundly affect the intangible qualities that make a person who they are. Recovery is complicated and highly dependent on the severity of the injury, a patient’s age and health, as well as the resources they have access to.
Ben’s sudden decline, while shocking to those who loved him, was in line with what much of the evidence suggests about these kinds of injuries: there is not one single, uniform path to recovery. Things can get incredibly complicated before they get better.
The team in the Trauma & Neurosurgery Inpatient Unit at St. Michael’s is about as interdisciplinary as they come. It’s like a hospital within a hospital, a specialized critical care unit that provides care to patients suffering from severe traumatic injuries or neurological conditions. Nurses, occupational and physical therapists, surgeons, physicians, speech and language specialists, and many more, work together to achieve the best outcomes for patients.
Dr. Najma Ahmed, a trauma surgeon, Surgeon-and-Chief at St. Michael’s Hospital, and Interim Chief Medical Officer at Unity Health, says “indefatiguable dedication coupled with innovative surgical approaches is the magic that makes such incredible outcomes possible.”
“It’s truly unbelievable, at least at St. Mike’s, how much like family you feel when you’re staying there,” Ben says. “I can’t describe it in words.”
Ultimately, after coming back to the St. Michael’s Trauma & Neurosurgery Inpatient Unit, Ben would need surgery to have a titanium mesh plate put in to act as a replacement skull. It was the first of many hurdles that Ben and Katherine would have to overcome, and the teams in at St. Michael’s were just getting started.
Read part two of Ben and Katherine’s story tomorrow, Thursday March 19.
Additional photos and video footage courtesy of Katherine Smith
