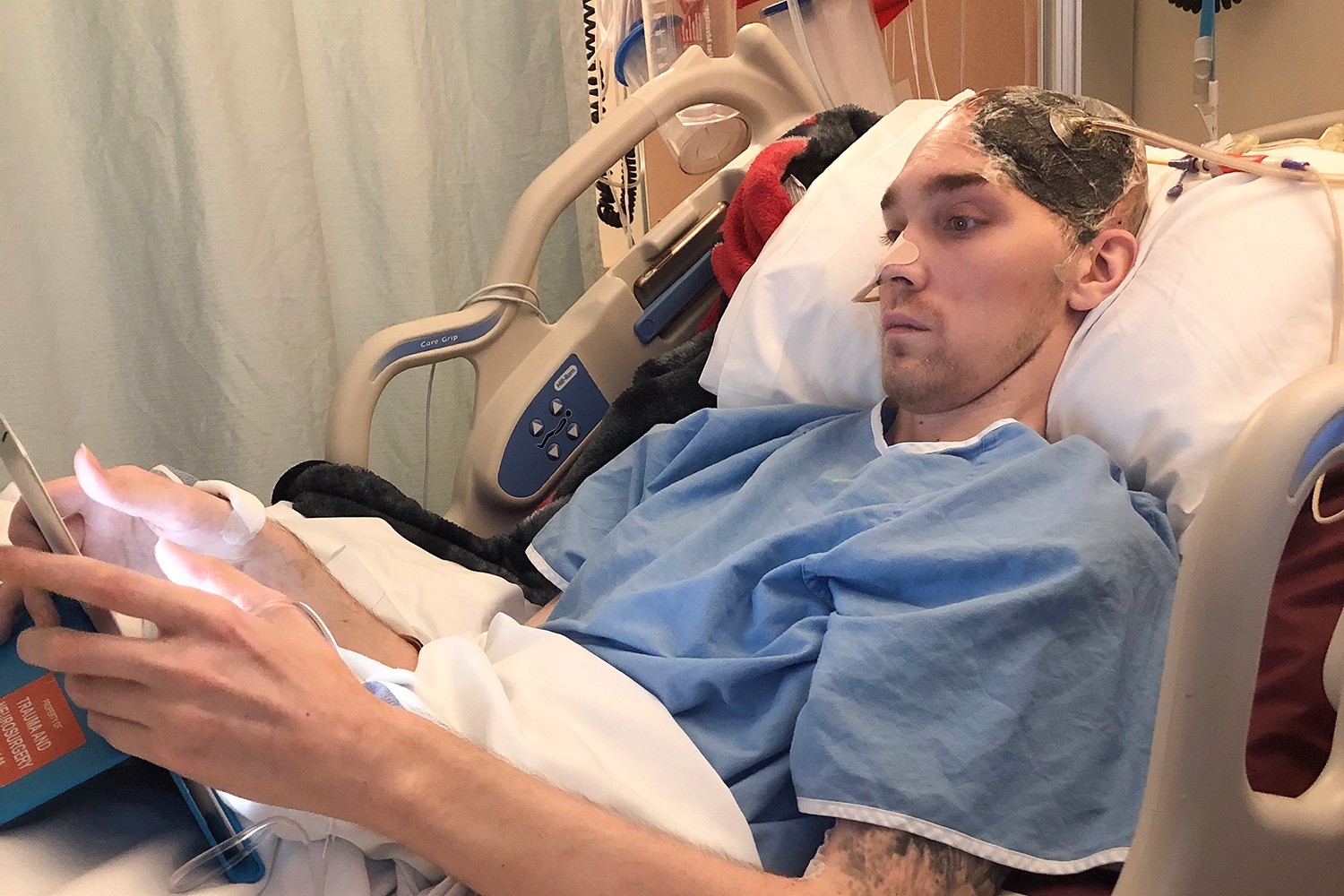
How personalized care gave a patient confidence after a traumatic brain injury
BY OLIVIA LAVERY
VIDEO AND PHOTOS BY KEVIN VAN PAASSEN
Read part one of Ben’s story to learn about the events that led to his arrival at St. Michael’s Hospital.
Personalized care centres around a patient and their unique needs. It gives them and their caregivers agency and control in their health care experience through shared decision making and empowerment, even in a scenario as precarious as Ben Finlan’s.
“They approach every case so differently,” Ben says of the personalized care his team offered to him at St. Michael’s Hospital. “It’s not one size fits all.”
Setting goals for recovery
Katherine Smith, Ben’s girlfriend, developed close relationships with his care team and kept detailed, handwritten logs of Ben’s condition and improvements. She became so attuned to his care that she could tell how he was feeling by how much he was able to open his eyes on any given day. Her notes highlight the most inspiring and challenging moments of their ordeal, like the day Ben was able to sit up on his own for the first time, when he struggled to eat and lost weight dangerously, or when COVID-19 restrictions prevented her from visiting. She was, in many ways, Ben’s voice during the time when he couldn’t use his own.
Ben’s care team recognized how important it was to keep him mentally and physically engaged in the recovery process.
Enjoying this story? Sign up for the Unity Health Toronto newsletter, a monthly update on the latest news, stories, patient voices and research emailed directly to subscribers.
During Ben’s first year at St. Michael’s Hospital, his physiotherapist Verity Tulloch spent a lot of time focusing on things like stretching. He wasn’t able to get in and out of bed yet, but there were still ways to keep him moving. Tulloch, knowing that Ben had been very active and athletic before the injury, developed activities and therapies geared towards sports to keep him motivated and engaged.
“Towards the third year we were able to get Ben sitting up on the end of the bed. We’d get him to sit for five to ten seconds,” says Tulloch.
Eventually he was able to practice standing up. Despite being young, Ben had lost a lot of bone density. One of the first times he tried to stand up, he broke a toe. It didn’t stop him for long. As Tulloch puts it, Ben never lost his fight.

Martha Miller, one of Ben’s occupational therapists, says a great deal of her work with patients revolves around goal setting; figuring out the things that mean the most to them that they want to work towards. Ben had specific goals in mind: playing 18 holes of golf and becoming a motivational speaker.
His occupational and physical therapists had to get creative. They found Ben a grip trainer so he could build up his hand strength and wrist movement to hold a golf club. Speech therapists guided him through the complicated and often exhausting process of learning to speak and communicate again.
“It’s step by step,” says Ben. “You have to start at the bottom and take it one day at a time.”
As Ben’s tolerance for sitting upright, reading and looking at a screen improved, Miller worried that he would get bored and decided to introduce him to online learning platforms. He started taking courses, and when he completed them he hung the certificates and diplomas in his room.
He says that the belief his care team had in him, and the confidence they had in his ability to learn and improve was very meaningful.
“You’re learning something new every day,” says Ben. “Instead of me sitting and watching TV shows and movies all day, she was actually trying to work with me and make me better than I was before I checked in.”
A final hurdle before rehab
His care required collaboration between so many departments that there is almost no area of the hospital it didn’t reach: orthopaedics, medical imaging, plastic surgery, neurosurgery, general surgery, anaesthesia, and more.
Dr. Blake Murphy is a plastic surgeon at St. Michael’s with expertise in craniofacial surgery and cancer reconstruction. He helps people who have been through devastating injury and illness to not only heal, but start to look and feel like themselves again.
Video: Ben’s story, part II
“One of the things that stood out to me most was how positive and resilient they both were,” says Dr. Murphy of Ben and Katherine. “It was pretty amazing to see someone who had been through such a long journey stay positive.”
Dr. Murphy’s role was to put together an interdisciplinary team of plastic surgeons, neurosurgeons, general surgeons, nurses and more to complete Ben’s final scalp reconstruction.
To reconstruct the scalp, Dr. Murphy’s team would need to take tissue from Ben’s abdomen, and transplant it to his scalp. To heal properly, this flap of tissue would have to be intricately connected to the existing blood vessels on Ben’s head. But, Ben had very few viable blood vessels. Even a small problem with the tissue overlying Ben’s reconstructed skull could cause major issues.
The team was able to complete the complex procedure, clearing one of the final hurdles to get Ben out of the hospital.
On his 32nd birthday, Ben was finally well enough to celebrate with friends and family outside, on the church lawn across the street from St. Michael’s. He was inching closer to going home.

Editor’s note: These stories reflect only a small portion of the many staff, physicians, teams, and departments involved in Ben’s care, and in the care of other patients like him. Read part one of the story here, and part three to learn more about Ben, Katherine, and the people who cared for them.
Additional photos and video footage courtesy of Katherine Smith
